Fracture & Trauma care
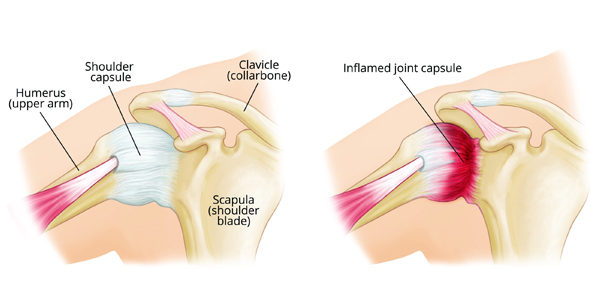
Frozen shoulder
Frozen Shoulder, also known as adhesive capsulitis, is a painful condition characterized by stiffness and restricted movement of the shoulder joint. It develops when the connective tissue surrounding the shoulder joint becomes inflamed and thickened, leading to progressive loss of mobility. Frozen shoulder commonly affects individuals between the ages of 40 and 60 and is more prevalent in people with diabetes, thyroid disorders, or those who have had prolonged shoulder immobilization after injury or surgery.
An Orthopaedic Surgeon plays a crucial role in diagnosing and treating frozen shoulder. Diagnosis is based on clinical examination, medical history, and imaging studies such as X-rays or MRI to rule out other shoulder conditions. Frozen shoulder typically progresses through three stages: the freezing stage, marked by increasing pain; the frozen stage, where stiffness limits movement; and the thawing stage, during which mobility gradually improves.
Treatment focuses on relieving pain and restoring shoulder movement. In the early stages, non-surgical management is often effective and may include pain-relieving medications, anti-inflammatory drugs, corticosteroid injections, and structured physical therapy. Stretching and range-of-motion exercises are essential to prevent further stiffness and improve flexibility. Heat therapy and guided rehabilitation may also help reduce discomfort.
When conservative treatment fails to provide adequate relief, an Orthopaedic Surgeon may recommend advanced interventions such as manipulation under anesthesia or arthroscopic capsular release. These minimally invasive procedures help loosen the tight joint capsule and improve shoulder mobility.
With timely diagnosis and appropriate care, most patients recover well from frozen shoulder. An experienced Orthopaedic Surgeon aims to reduce pain, restore functional movement, and help patients return to their daily activities comfortably and confidently.

